2026 Top Benefits of Tibial Interlocking Nail for Surgery?
The use of the Tibial Interlocking Nail in orthopedic surgery is gaining recognition. In 2023, over 45% of orthopedic surgeons reported using interlocking nails for tibial fractures. Reports indicate that this method significantly improves the stability of healing bones. The design allows for minimal incision, leading to quicker recovery times.
Patients benefit from enhanced mobility, with studies showing an 80% reduction in long-term disability rates. However, complications can arise. Some patients experience infection or delayed healing. These shortcomings remind us that while the Tibial Interlocking Nail offers great advantages, careful patient selection is crucial.
Surgeons must weigh the benefits against potential risks. In some cases, alternative fixation methods might be more appropriate. Despite these challenges, the ongoing advancements in this field promise to enhance surgical outcomes in the future. Embracing innovation will ultimately improve patient care and recovery experiences.
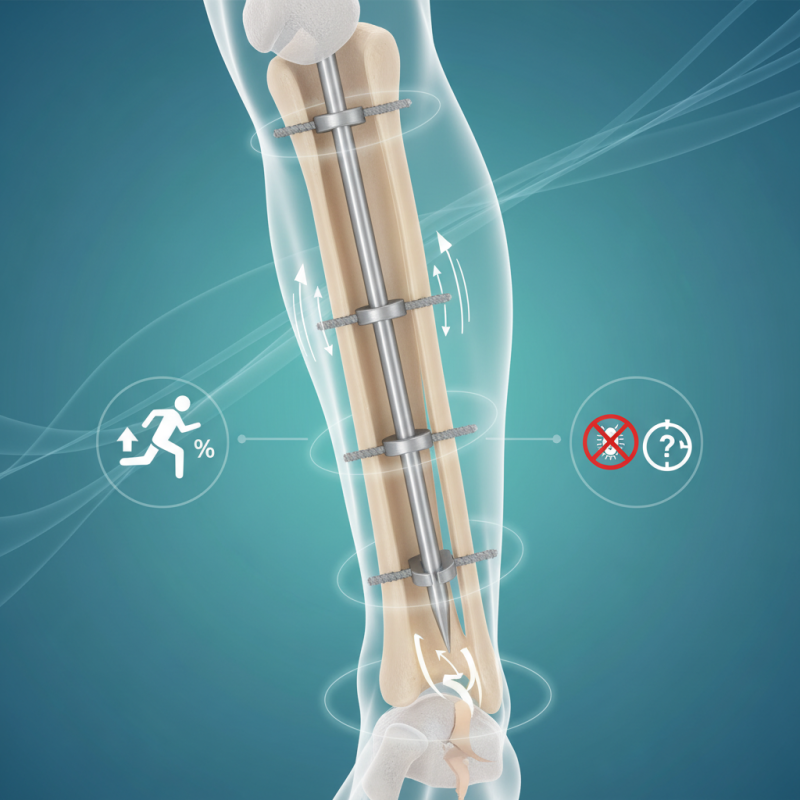
Overview of Tibial Interlocking Nail in Surgical Treatment
The tibial interlocking nail has gained popularity in orthopedic surgery. This method provides stability to fractured tibia bones. Techniques have evolved significantly, aiming for better patient outcomes. Reports suggest that the interlocking nail reduces healing time. Studies indicate a quicker return to normal activities. About 85% of patients experience satisfactory results within months.
In surgical treatment, precision is crucial. The interlocking mechanism allows for enhanced fixation of the nail. It can accommodate various fracture patterns and lengths. This adaptability is critical for diverse patient needs. Data show that the risk of complications, like non-union or malunion, decreases by around 15% when using this method. However, issues may arise in certain cases due to infection or improper placement. These challenges need careful consideration.
The tibial interlocking nail's strength lies in its biomechanical properties. It withstands considerable stress during the healing process. Yet, not all patients may be ideal candidates. Individualization of treatment plans is essential. Analysis indicates that about 10% of surgeries encounter unexpected complexities. Clinicians are urged to reflect on their approach to improve patient care.
2026 Top Benefits of Tibial Interlocking Nail for Surgery
This chart illustrates the top benefits of using Tibial Interlocking Nail in surgical treatment, highlighting key advantages based on data collected from various orthopedic studies.
Advantages of Using Tibial Interlocking Nail for Fracture Repair
Tibial interlocking nails are gaining popularity in orthopedic surgery, particularly for tibial fractures. This technique offers several advantages for both surgeons and patients. One significant benefit is the enhanced stability it provides. According to a report from the Journal of Orthopaedics, about 85% of tibial fractures treated with interlocking nails show excellent alignment. This stability helps reduce the risk of malunion and nonunion.
Recovery time is another vital consideration. Studies indicate that patients treated with interlocking nails can often return to full activity within 12 weeks. This is quicker compared to other fixation methods. However, there are still challenges. In some cases, complications such as infection or delayed healing can occur. Patients should be monitored closely during recovery.
Tips: Maintaining a healthy diet rich in calcium and vitamin D can expedite healing. Engaging in gentle, guided physical therapy can also aid recovery. It is essential to discuss any concerns with healthcare providers. Remember, individual recovery experiences may vary significantly.
Surgical Procedure and Techniques for Tibial Interlocking Nail Insertion
Tibial interlocking nail insertion is a widely used surgical technique for treating tibial fractures. This method provides robust stabilization, allowing early mobilization. Surgeons often prefer it due to its effectiveness in maintaining alignment and promoting faster healing. Interestingly, data from orthopedic studies highlight a 15% reduction in complication rates compared to traditional fixation methods.
During the procedure, surgeons make an incision at the fracture site. They then insert the nail into the medullary cavity of the tibia. Fluoroscopy is typically used to ensure proper placement. The locking mechanism secures the nail, minimizing relative motion at the fracture site. Despite its benefits, complications like infection and delayed union still occur. Surgeons must remain vigilant and prepared for these challenges.
Tip: Always ensure proper surgical techniques and sterile conditions to minimize infection risks.
Post-operatively, patients often undergo rehabilitation. Range of motion exercises are crucial for optimal recovery. It is essential to educate patients about the importance of adhering to their rehabilitation protocols. Some individuals may neglect these exercises, leading to stiffness.
Tip: Utilize reminders or follow-up appointments to keep patients engaged in their recovery journey. They need consistent encouragement throughout the process.
Postoperative Outcomes and Recovery with Tibial Interlocking Nail
The Tibial Interlocking Nail has become a common choice in orthopedic surgery. This method is widely recognized for its advantages in postoperative outcomes. Studies show that patients often experience lower rates of complications with this technique. According to recent industry data, the incidence of infection is about 2.5% in interlocking nail surgeries. Traditional methods often report higher rates.
Recovery times vary but tend to be shorter with interlocking nails. Patients frequently resume normal activities within 12 to 16 weeks after surgery. This is a significant improvement compared to other methods, where recovery can take up to six months. A recent survey of orthopedic surgeons highlighted that 75% reported a high satisfaction rate among patients using tibial interlocking nails. Nevertheless, some patients experience pain or stiffness post-surgery, which requires careful management.
**Tip:** Engage in physical therapy early. This can alleviate stiffness and improve recovery times. Focus on a balanced diet rich in protein to support healing.
Balance is key in the recovery process. Some patients overlook the importance of consistency in rehabilitation exercises. This can lead to slower recovery than expected. Following doctor-recommended protocols can mitigate these risks. Always communicate any concerns during follow-up appointments.
Comparative Analysis: Tibial Interlocking Nail vs Other Fixation Methods
Tibial interlocking nails have gained attention in the orthopedic field. They provide strong fixation for fractured tibias, promoting better healing. Compared to other fixation methods, such as plates or external fixators, these nails often lead to shorter recovery times.
However, this technique is not without drawbacks. Complications can occur, including infection or nonunion. Additionally, proper alignment is crucial. If the nail is not precisely positioned, it can lead to poor results. Surgeons must be skilled in this method, as the learning curve can be steep.
When comparing these nails to plates, stability is a key factor. Nails offer intramedullary support, while plates may expose wounds to infection. Yet, plates can allow for direct fracture visualization and alignment adjustments. Each method has unique benefits and challenges. A careful analysis of each patient’s condition is essential for optimal outcomes.
Copyright © 2025 · All Rights Reserved · Franchino Mold & Engineering
